Stress & hair loss science is a subject I discuss frequently during consultations. Many patients ask, “I’ve been under significant stress, could that be why my hair is falling out?” The answer is yes, stress can influence hair growth. However, the process is biological and often delayed, which can make it confusing. Hair follicles are …
Stress & hair loss science is a subject I discuss frequently during consultations. Many patients ask, “I’ve been under significant stress, could that be why my hair is falling out?”
The answer is yes, stress can influence hair growth. However, the process is biological and often delayed, which can make it confusing.
Hair follicles are highly responsive structures. They react not only to hormones and nutrition, but also to internal stress signals. Understanding how stress interacts with the hair growth cycle helps distinguish temporary shedding from more persistent forms of hair loss.
What Is Stress-Related Hair Loss?
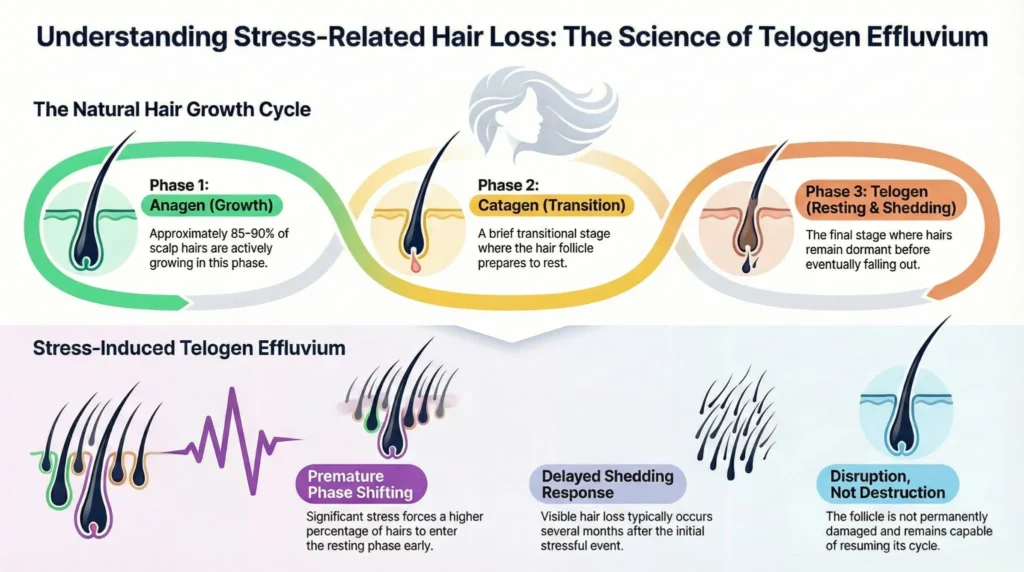
To understand stress-related shedding, it helps to revisit the hair growth cycle. Each follicle moves independently through three stages:
- Anagen (growth phase)
- Catagen (transition phase)
- Telogen (resting and shedding phase)
Normally, around 85–90% of scalp hairs are in the growth phase at any given time. When the body experiences significant stress, a higher proportion of hairs can shift prematurely into the resting phase.
Several months later, those hairs shed.
This condition is known as telogen effluvium.
Importantly, the follicle itself is not usually permanently damaged. The cycle has been disrupted, not destroyed.
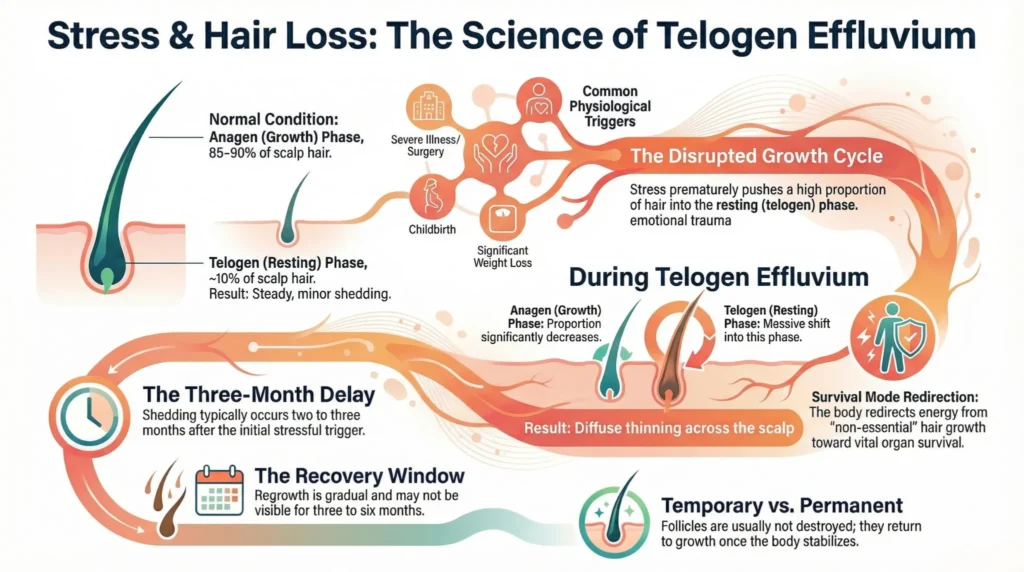
How Does Stress Affect the Hair Follicle?
When the body is under stress, it releases hormones such as cortisol and adrenaline. These are part of the natural “fight or flight” response. In short bursts, they are protective.
However, prolonged or intense stress can disturb biological balance.
Research suggests stress may:
- Alter hormone regulation
- Increase inflammatory signalling
- Influence blood flow to follicles
- Affects immune system activity
Hair is not essential for survival. When the body is under strain, energy is redirected towards vital organs. As a result, the hair growth phase may shorten.
One important point: shedding rarely occurs immediately after a stressful event. There is often a delay of two to three months. This timing gap can make it difficult to identify the original trigger.
Types of Stress That Can Trigger Hair Loss
Stress is not limited to emotional strain. The body interprets many events as physiological stressors.
Common triggers include:
- Severe illness or high fever
- Surgery
- Childbirth
- Significant weight loss
- Emotional trauma
- Prolonged anxiety
- Major life changes
Even positive events can create enough physical strain to disrupt the hair cycle.
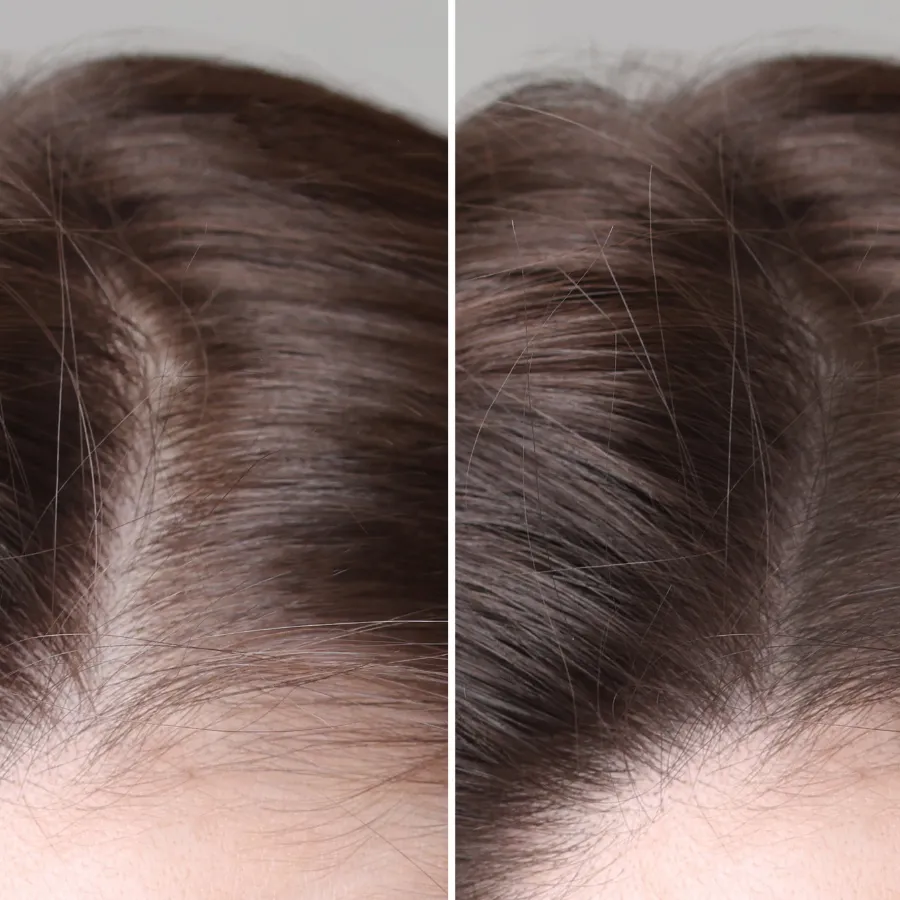
What Does Stress-Related Hair Loss Look Like?
In most cases, stress-related shedding presents as diffuse thinning. This means the hair appears thinner across the entire scalp rather than in a specific pattern.
Patients often report:
- Increased hair in the shower
- More strands on pillows or clothing
- Excess shedding when brushing
- Reduced ponytail thickness
- A general decrease in volume
The scalp typically appears healthy. There are no clear bald patches and usually no visible inflammation.
If hair loss becomes patchy or the scalp feels painful or inflamed, other causes should be considered.
Is Stress Hair Loss Permanent?
In the majority of cases, telogen effluvium is temporary.
Once the underlying stress resolves and the body stabilises, follicles gradually return to the growth phase. However, recovery takes time.
Because of the natural length of the hair cycle, regrowth may not be noticeable for three to six months. Full improvement may take longer depending on the individual.
If underlying genetic thinning is present, stress-related shedding may make it appear more pronounced. In these situations, both contributing factors need to be evaluated.
How Is Stress-Related Hair Loss Assessed?
Assessment always begins with history and timing. If shedding begins approximately three months after illness, surgery, or emotional strain, the pattern often aligns with telogen effluvium.
During examination, I assess:
- Overall hair density
- Distribution of thinning
- Variation in hair shaft diameter
- Scalp health
This helps distinguish stress-related shedding from genetic pattern hair loss or inflammatory scalp conditions.
Where appropriate, I may suggest discussing blood tests with a GP to rule out iron deficiency or thyroid imbalance, as these can also influence the hair cycle.
The aim is to determine whether stress is the primary trigger or part of a broader clinical picture.
What Can Support Recovery?
There is no immediate treatment that reverses stress-related shedding overnight. The body requires time to re-establish balance.
Supportive measures may include:
- Managing stress levels where possible
- Maintaining balanced nutrition
- Prioritising sleep
- Treating any underlying scalp conditions
- Monitoring changes over time
Aggressive treatment is rarely necessary for straightforward telogen effluvium. In many cases, reassurance and structured monitoring are appropriate.
If shedding continues beyond six months, further evaluation is advisable.
When Should You Seek Advice?
Professional assessment may be helpful if:
- Shedding persists for more than three to six months
- Thinning appears progressive
- Hair loss becomes patchy
- The scalp feels persistently sore or inflamed
Not all shedding requires intervention. However, understanding the cause often provides clarity and reassurance.
Patients who attend The Hair & Scalp Clinic in Huntingdon receive a detailed, evidence-based scalp assessment with Consultant Trichologist Tracey Walker FIT. The focus is always on identifying the underlying trigger before discussing management options.
Stress can influence the hair growth cycle, but in many cases, the process is reversible. With careful assessment, realistic expectations, and calm guidance, most individuals can understand what is happening and what, if anything, needs to be done.